Abstract
SIRT6, a member of the NAD(+)-dependent class III deacetylase sirtuin family, has been revealed to play important roles in promoting cellular resistance against oxidative stress. The formation of reactive oxygen species (ROS) and oxidative stress are the crucial mechanisms underlying cellular damage and dysfunction in cardiac ischemia/reperfusion (I/R) injury, but the role of SIRT6 in I/R-induced ROS and oxidative stress is poorly understood. In this study, by using heterozygous SIRT6 knockout (SIRT6+/−) mice and cultured neonatal cardiomyocyte models, we investigated how SIRT6 mediates oxidative stress and myocardial injury during I/R. Partial knockout (KO) of SIRT6 aggravated myocardial damage, ventricular remodeling, and oxidative stress in mice subjected to myocardial I/R, whereas restoration of SIRT6 expression by direct cardiac injection of adenoviral constructs encoding SIRT6 reversed these deleterious effects of SIRT6 KO in the ischemic heart. In addition, partial deletion of the SIRT6 gene decreased myocardial functional recovery following I/R in a Langendorff perfusion model. Similarly, the protective effects of SIRT6 were also observed in cultured cardiomyocytes following hypoxia/reoxygenation. Intriguingly, SIRT6 was noticed to up-regulate AMP/ATP and then activate the adenosine 5′-monophosphate-activated protein kinase (AMPK)-forkhead box O3α (FoxO3α) axis and further initiated the downstream antioxidant-encoding gene expression (manganese superoxide dismutase and catalase), thereby decreasing cellular levels of oxidative stress and mediating cardioprotection in the ischemic heart. These results suggest that SIRT6 protects the heart from I/R injury through FoxO3α activation in the ischemic heart in an AMP/ATP-induced AMPK-dependent way, thus upregulating antioxidants and suppressing oxidative stress.








Similar content being viewed by others
References
Murphy E, Steenbergen C (2008) Mechanisms underlying acute protection from cardiac ischemia-reperfusion injury. Physiol Rev 88:581–609. doi:10.1152/physrev.00024.2007
Eltzschig HK, Eckle T (2011) Ischemia and reperfusion-from mechanism to translation. Nat Med 17:1391–1401. doi:10.1038/nm.2507
Goswami SK, Maulik N, Das DK (2007) Ischemia-reperfusion and cardioprotection: a delicate balance between reactive oxygen species generation and redox homeostasis. Ann Med 39:275–289. doi:10.1080/07853890701374677
Heusch G (2015) Molecular basis of cardioprotection: signal transduction in ischemic pre-, post-, and remote conditioning. Circ Res 13(116):674–699. doi:10.1161/CIRCRESAHA.116.305348
Tullio F, Angotti C, Perrelli MG, Penna C, Pagliaro P (2013) Redox balance and cardioprotection. Basic Res Cardiol 108(6):392. doi:10.1007/s00395-013-0392-7
Ahn YJ, Kim H, Lim H, Lee M, Kang Y, Moon S, Kim HS, Kim HH (2012) AMP-activated protein kinase: implications on ischemic diseases. BMB Rep 45:489–495. doi:10.5483/BMBRep.2012.45.9.169
Koentges C, König A, Pfeil K, Hölscher ME, Schnick T, Wende AR, Schrepper A, Cimolai MC, Kersting S, Hoffmann MM, Asal J, Osterholt M, Odening KE, Doenst T, Hein L, Abel ED, Bode C, Bugger H (2015) Myocardial mitochondrial dysfunction in mice lacking adiponectin receptor 1. Basic Res Cardiol 110:37. doi:10.1007/s00395-015-0495-4
Koentges C, Pfeil K, Schnick T, Wiese S, Dahlbock R, Cimolai MC, Meyer-Steenbuck M, Cenkerova K, Hoffmann MM, Jaeger C, Odening KE, Kammerer B, Hein L, Bode C, Bugger H (2015) SIRT3 deficiency impairs mitochondrial and contractile function in the heart. Basic Res Cardiol 110:36. doi:10.1007/s00395-015-0493-6
Yang Y, Duan W, Li Y, Jin Z, Yan J, Yu S, Yi D (2013) Novel role of silent information regulator 1 in myocardial ischemia. Circulation 128:2232–2240. doi:10.1161/CIRCULATIONAHA.113.002480
Hall JA, Dominy JE, Lee Y, Puigserver P (2013) The sirtuin family’s role in aging and age-associated pathologies. J Clin Invest 123:973–979. doi:10.1172/JCI64094
Sebastián C, Satterstrom FK, Haigis MC, Mostoslavsky R (2012) From sirtuin biology to human diseases: an update. J Biol Chem 287:42444–42452. doi:10.1074/jbc.R112.402768
Beauharnois JM, Bolívar BE, Welch JT (2013) Sirtuin 6: a review of biological effects and potential therapeutic properties. Mol BioSyst 9:1789–1806. doi:10.1039/c3mb00001j
Sundaresan NR, Vasudevan P, Zhong L, Kim G, Samant S, Parekh V, Pillai VB, Ravindra PV, Gupta M, Jeevanandam V, Cunningham JM, Deng CX, Lombard DB, Mostoslavsky R, Gupta MP (2012) The sirtuin SIRT6 blocks IGF-Akt signaling and development of cardiac hypertrophy by targeting c-Jun. Nat Med 18:1643–1650. doi:10.1038/nm.2961
Mao Z, Hine C, Tian X, Van Meter M, Au M, Vaidya A, Seluanov A, Gorbunova V (2011) SIRT6 promotes DNA repair under stress by activating PARP1. Science 332:1443–1446. doi:10.1126/science.1202723
Chiang WC, Tishkoff DX, Yang B, Wilson-Grady J, Yu X, Mazer T, Eckersdorff M, Gygi SP, Lombard DB, Hsu AL (2012) C. elegans SIRT6/7 homolog SIR-2.4 promotes DAF-16 relocalization and function during stress. PLoS Genet 8:e1002948. doi:10.1371/journal.pgen.1002948
Ronnebaum SM, Patterson C (2010) The FoxO family in cardiac function and dysfunction. Annu Rev Physiol 72:81–94. doi:10.1146/annurev-physiol-021909-135931
Accili D, Arden KC (2004) FoxOs at the crossroads of cellular metabolism, differentiation, and transformation. Cell 117:421–426. doi:10.1016/S0092-8674(04)00452-0
Tao R, Xiong X, DePinho RA, Deng CX, Dong XC (2013) FoxO3 transcription factor and Sirt6deacetylase regulate low density lipoprotein (LDL)-cholesterol homeostasis via control of the proprotein convertase subtilisin/kexin type 9 (Pcsk9) gene expression. J Biol Chem 288:29252–29259. doi:10.1074/jbc.M113.481473
Zhong L, D’Urso A, Toiber D, Sebastian C, Henry RE, Vadysirisack DD, Guimaraes A, MarinelliB Wikstrom JD, Nir T, Clish CB, Vaitheesvaran B, Iliopoulos O, Kurland I, Dor Y, Weissleder R, Shirihai OS, Ellisen LW, Espinosa JM, Mostoslavsky R (2010) The histone deacetylase Sirt6 regulates glucose homeostasis via Hif1alpha. Cell 140:280–293. doi:10.1016/j.cell
Pachori AS, Melo LG, Zhang L, Solomon SD, Dzau VJ (2006) Chronic recurrent myocardial ischemic injury is significantly attenuated by pre-emptive adeno-associated virus hemeoxygenase-1 gene delivery. J Am Coll Cardiol 47:635–643. doi:10.1016/j.jacc.2005.09.038
Jiang W, Hall SR, Moos MP, Cao RY, Ishii S, Ogunyankin KO, Melo LG, Funk CD (2008) Endothelial cysteinyl leukotriene 2 receptor expression mediates myocardial ischemia-reperfusion injury. Am J Pathol 172:592–602. doi:10.2353/ajpath
Chen H, Wang X, Tong M, Wu D, Wu S, Chen J, Wang X, Wang X, Kang Y, Tang H, Tang C, Jiang W (2013) Intermedin suppresses pressure overload cardiac hypertrophy through activation of autophagy. PLoS One 8:e64757. doi:10.1371/journal
Liu X, Simpson JA, Brunt KR, Ward CA, Hall SR, Kinobe RT, Barrette V, Tse MY, Pang SC, Pachori AS, Dzau VJ, Ogunyankin KO, Melo LG (2007) Preemptive heme oxygenase-1 gene delivery reveals reduced mortality and preservation of left ventricular function 1 year after acute myocardial infarction. Am J Physiol Heart Circ Physiol 293:H48–H59. doi:10.1152/ajpheart.00741.2006
Hsu CP, Zhai P, Yamamoto T, Maejima Y, Matsushima S, Hariharan N, Shao D, Takagi H, Oka S, Sadoshima J (2010) Silent information regulator 1 protects the heart from ischemia/reperfusion. Circulation 122:2170–2182. doi:10.1161/CIRCULATIONAHA.110.958033
Yang Y, Duan W, Lin Y, Yi W, Liang Z, Yan J, Wang N, Deng C, Zhang S, Li Y, Chen W, Yu S, YiD Jin Z (2013) SIRT1 activation by curcumin pretreatment attenuates mitochondrial oxidative damage induced by myocardial ischemia reperfusion injury. Free Radic Biol Med 65:667–679. doi:10.1016/j.freeradbiomed
Shibata R, Sato K, Pimentel DR, Takemura Y, Kihara S, Ohashi K, Funahashi T, Ouchi N, Walsh K (2005) Adiponectin protects against myocardial ischemia–reperfusion injury through AMPK and COX-2-dependent mechanisms. Nat Med 11:1096–1103. doi:10.1038/nm1295
Zafir A, Readnower R, Long BW, McCracken J, Aird A, Alvarez A, Cummins TD, Li Q, Hill BG, Bhatnagar A, Prabhu SD, Bolli R, Jones SP (2013) Protein O-GlcNAcylation is a novel cytoprotective signal in cardiac stem cells. Stem Cells 31:765–775. doi:10.1002/stem.1325
Sundaresan NR, Gupta M, Kim G, Rajamohan SB, Isbatan A, Gupta MP (2009) Sirt3 blocks the cardiac hypertrophic response by augmenting Foxo3a-dependent antioxidant defense mechanisms in mice. J Clin Invest 119:2758–2771. doi:10.1172/JCI39162
Wang X, Wang XL, Chen HL, Wu D, Chen JX, Wang XX, Li RL, He JH, Mo L, Cen X, Wei YQ, Jiang W (2014) Ghrelin inhibits doxorubicin cardiotoxicity by inhibiting excessive autophagy through AMPK and p38-MAPK. Biochem Pharmacol 88:334–350. doi:10.1016/j.bcp.2014.01.040
Bhatt DP, Chen X, Geiger JD, Rosenberger TA (2012) A sensitive HPLC-based method to quantify adenine nucleotides in primary astrocyte cell cultures. J Chromatogr B Analyt Technol Biomed Life Sci 889–890:110–115. doi:10.1016/j.jchromb
Funai K, Song H, Yin L, Lodhi IJ, Wei X, Yoshino J, Coleman T, Semenkovich CF (2013) Muscle lipogenesis balances insulin sensitivity and strength through calcium signaling. J Clin Invest 123:1229–1240. doi:10.1172/JCI65726
Brunet A, Sweeney LB, Sturgill JF, Chua KF, Greer PL, Lin Y, Tran H, Ross SE, Mostoslavsky R, Cohen HY, Hu LS, Cheng HL, Jedrychowski MP, Gygi SP, Sinclair DA, Alt FW, Greenberg ME (2004) Stress-dependent regulation of FOXO transcription factors by the SIRT1 deacetylase. Science 303:2011–2015. doi:10.1126/science.1094637
Li Z, Zhang H, Chen Y, Fan L, Fang J (2012) Forkhead transcription factor FOXO3a protein activates nuclear factor κB through B-cell lymphoma/leukemia 10 (BCL10) protein and promotes tumor cell survival in serum deprivation. J Biol Chem 18(287):17737–17745. doi:10.1074/jbc.M111.291708
Olmos Y, Sánchez-Gómez FJ, Wild B, García-Quintans N, Cabezudo S, Lamas S, Monsalve M (2013) SirT1 regulation of antioxidant genes is dependent on the formation of a FoxO3a/PGC-1α complex. Antioxid Redox Signal 19:1507–1521. doi:10.1089/ars.2012.4713
Heusch G, Libby P, Gersh B, Yellon D, Böhm M, Lopaschuk G, Opie L (2014) Cardiovascular remodeling in coronary artery disease and heart failure. Lancet 383:1933–1943. doi:10.1016/S0140-6736(14)60107-0
Hardie DG, Ross FA, Hawley SA (2012) AMPK: a nutrient and energy sensor that maintains energy homeostasis. Nat Rev Mol Cell Biol 13:251–262. doi:10.1038/nrm3311
Greer EL, Banko MR, Brunet A (2009) AMP-activated protein kinase and FoxO transcription factors in dietary restriction-induced longevity. Ann N Y Acad Sci 1170:688–692. doi:10.1111/j.1749-6632
Chiacchiera F, Simone C (2010) The AMPK–FoxO3A axis as a target for cancer treatment. Cell Cycle 9:1091–1096. doi:10.4161/cc.9.6.11035
Sengupta A, Kalinichenko VV, Yutzey KE (2013) FoxO1 and FoxM1 transcription factors have antagonistic functions in neonatal cardiomyocyte cell-cycle withdrawal and IGF1 gene regulation. Circ Res 112:267–277. doi:10.1161/CIRCRESAHA.112.277442
Lopaschuk GD, Stanley WC (1997) Glucose metabolism in the ischemic heart. Circulation 95:313–315. doi:10.1161/01.CIR.95.2.313
Rosano GM, Fini M, Caminiti G, Barbaro G (2008) Cardiac metabolism in myocardial ischemia. Curr Pharm Des 14:2551–2562. doi:10.2174/138161208786071317
Wang P, Tate JM, Lloyd SG (2008) Low carbohydrate diet decreases myocardial insulin signaling and increases susceptibility to myocardial ischemia. Life Sci 83:836–844. doi:10.1016/j.lfs.2008.09.024
Maksin-Matveev A, Kanfi Y, Hochhauser E, Isak A, Cohen HY, Shainberg A (2015) Sirtuin 6 protects the heart from hypoxic damage. Exp Cell Res 330:81–90. doi:10.1016/j.yexcr.2014.07.013
Sengupta A, Molkentin JD, Paik JH, DePinho RA, Yutzey KE (2011) FoxO transcription factors promote cardiomyocyte survival upon induction of oxidative stress. J Biol Chem 286:7468–7478. doi:10.1074/jbc.M110.179242
Li X, Wang L, Zhou XE, Ke J, de Waal PW, Gu X, Tan MH, Wang D, Wu D, Xu HE, Melcher K (2015) Structural basis of AMPK regulation by adenine nucleotides and glycogen. Cell Res 25:50–66. doi:10.1038/cr.2014.150
Kudo N, Gillespie JG, Kung L, Witters LA, Schulz R, Clanachan AS, Lopaschuk GD (1996) Characterization of 5′AMP-activated protein kinase activity in the heart and its role in inhibiting acetyl-CoA carboxylase during reperfusion following ischemia. Biochim Biophys Acta 1301:67–75. doi:10.1016/0005-2760(96)00013-6
Kodiha M, Rassi JG, Brown CM, Stochaj U (2007) Localization of AMP kinase is regulated by stress, cell density, and signaling through the MEK–>ERK1/2 pathway. Am J Physiol Cell Physiol 293:C1427–C1436. doi:10.1152/ajpcell.00176.2007
Greer EL, Oskoui PR, Banko MR, Maniar JM, Gygi MP, Gygi SP, Brunet A (2007) The energy sensor AMP-activated protein kinase directly regulates the mammalian FOXO3 transcription factor. J Biol Chem 282:30107–30119. doi:10.1074/jbc.M705325200
Li XN, Song J, Zhang L, LeMaire SA, Hou X, Zhang C, Coselli JS, Chen L, Wang XL, Zhang Y, Shen YH (2009) Activation of the AMPK-FoxO3 pathway reduces fatty acid-induced increase in intracellular reactive oxygen species by upregulating thioredoxin. Diabetes 58:2246–2257. doi:10.2337/db08-1512
Acknowledgments
This work was supported by the National Natural Science Foundation of China (30871017, 31071001 and 31271226 to Dr. W Jiang).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Electronic supplementary material
Below is the link to the electronic supplementary material.
395_2016_531_MOESM1_ESM.tif
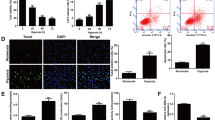
Supplementary Figure I. Effect of sirt6 on I/R injury in cardiac tissues and H/R damage in cardiomyocytes. A. L-lactate dehydrogenase (LDH), creatine kinase (CK) and MB isoenzyme of CK (CK-MB) activities in plasma of WT and SIRT6+/− mice 24 hours after I/R (n = 10/group). B-D. LDH, CK and CK-MB activities in perfusates of isolated WT and SIRT6+/− mouse hearts (n = 10/group), respectively. E and F. LDH, CK and CK-MB activities in cultural supernatants of mock or sirt6-siRNA transfected, or Ad-null or Ad-SIRT6 infected cardiomyocytes with 8 h of hypoxia followed by 2 h of reoxygenation (n = 7/group), respectively. G-I. LDH, CK and CK-MB activities in plasma of Ad-null or Ad-SIRT6 infected WT and SIRT6+/− mice 24 hours after I/R (n = 10/group). J-L. LDH, CK and CK-MB activities in cultural supernatants of mock or sirt6-siRNA transfected cardiomyocytes in the absence and presence of 10 µmol/L compound C or FoxO3α siRNA with 8 h of hypoxia followed by 2 h of reoxygenation (n = 7/group), respectively. Cardiac enzyme activities in plasma and cell culture supernatants were statistically analyzed with the one-way ANOVA, and in perfusates of isolated hearts with the unpaired Student’s t-test. *P < 0.05, **P < 0.01; in Figure B-D, *P < 0.05, **P < 0.01 vs WT control. (TIFF 11840 kb)
395_2016_531_MOESM2_ESM.tif
Supplementary Figure II. Effect of sirt6 on Left Ventricular Remodeling 4 weeks after cardiac I/R injury. A. Histomorphological appearance and remodeling of the LV 4 weeks after I/R. Hearts were sectioned at the level of the papillary muscles, and stained with Masson’s trichrome (the up panels, scale bar = 20 μm; the bottom panels, scale bar = 1 mm). B and C. Morphometric analysis of LV fibrosis (C) and wall thinning (D) in WT and SIRT6+/− animals (n = 6/group), respectively. D. Representative M-mode frames from the mid-papillary region of sham WT (a) and SIRT6+/− (c) mice, as well as infracted WT (b) and SIRT6+/− (d) mice 4 weeks after acute I/R injury. Yellow arrow indicates width of the LV chamber. LV fibrosis was statistically analyzed with the one-way ANOVA, and wall thinning with the unpaired Student’s t-test. *P < 0.05, **P < 0.01 (TIFF 18698 kb)
Rights and permissions
About this article
Cite this article
Wang, XX., Wang, XL., Tong, Mm. et al. SIRT6 protects cardiomyocytes against ischemia/reperfusion injury by augmenting FoxO3α-dependent antioxidant defense mechanisms. Basic Res Cardiol 111, 13 (2016). https://doi.org/10.1007/s00395-016-0531-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00395-016-0531-z